Non-Oncologic Vascular Procedures
Intrahepatic Portosystemic Shunts
Arteriovenous fistula/malformation
Intravascular Foreign Body Removal
Epistaxis (bleeding from the nostril)
IHPSS PTCE
Intrahepatic Portosystemic Shunts (IHPSS)
A portosystemic shunt is an abnormal connection between major blood vessels in the abdomen. This abnormal connection results in blood bypassing the liver and prevents the liver from performing blood filtering. Signs that may be noted in dogs and cats with portosystemic shunts include, but are not limited to, small body size, low energy level, mental dullness and seizures.
A minimally-invasive procedure has been developed in which coils are placed in the portosystemic shunt to allow the shunt to close down progressively over time. The coils are held in place by the use of a metal or metal-alloy stent. The entire procedure is performed through a small puncture in a blood vessel in the neck region. The goal of the procedure is to help the liver be able to perform normal functions more effectively as more blood travels through the liver.
AVM Embolization
Arteriovenous fistula / malformation
An arteriovenous fistula/malformation otherwise known as an AVF or AVM is an abnormal connection (or several) between an artery and a vein. This usually develops during pregnancy, however, trauma and surgery can also lead to the development of an AVF or AVM. Depending on the location of the AVF/AVM, your pet may experience an accumulation of fluid or a swelling. These fluid accumulations can cause discomfort or excessive pressure on surrounding tissue.
Some AVF/AVM can be eliminated by the placement of glue or other agents in the blood vessel to close down the communication. This procedure is not possible in all cases, but when it can be performed, dramatic improvement may occur.
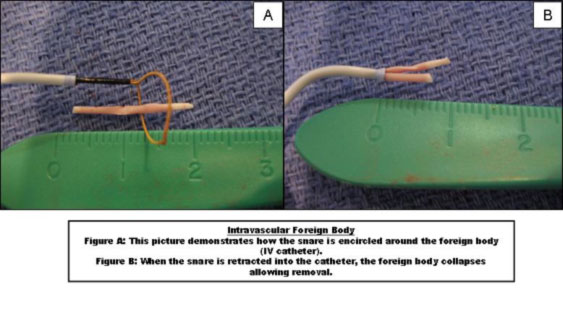 Intravascular Foreign Body Removal
Intravascular Foreign Body Removal
Intravenous (IV) catheters are commonly placed in dogs and cats for both elective and non-elective procedures. If an IV catheter is accidentally cut during removal, part of the catheter (“foreign body”) may launch into the patient’s circulatory system. No studies have been performed that document long-term side effects in these patients, however, severe complications have been documented in humans.
Prior to the implementation of IR techniques in veterinary patients, surgery was the only treatment option for removal of these intravascular foreign bodies. With the use of fluoroscopy and a snare that can be manipulated through the circulatory system, these foreign bodies can often be removed through a small incision.
Nasal Embolization
Epistaxis (bleeding from the nostril)
Nose bleeds (epistaxis) can develop from nasal trauma, cancer and inflammation, but on occasion, a nose bleed may develop from unknown causes (“idiopathic epistaxis”). The bleeding that occurs in these cases may be excessive, and can lead to life-threatening blood loss. In some of these cases, an agent can be injected through a catheter into the bleeding vessel to cause the vessel to occlude, thus preventing further bleeding. This procedure is performed through a very small incision, and post-procedure pain is very minimal.
