Benign Obstructions
Tracheal Stent
Tracheal Collapse
The trachea is a flexible tube in the neck and chest that allows passage of air down to the lungs during breathing. When the trachea loses rigidity, it can close down or "collapse" and prevent air movement to the lungs. This is often manifested by a "honking" cough, and signs such as blue gums and falling over may occur. Tracheal collapse is often worsened by conditions that cause your pet to become excited such as stress or exercise, hot weather, and eating or drinking. After the diagnosis has been confirmed, management with oral medications and weight control are generally recommended, but these may not always be successful. Surgery can be a treatment option for some pets with tracheal collapse; however, this is not recommended in all cases.
For dogs with tracheal collapse that is refractory to medical management, tracheal stenting may need to be considered; however, it is important to remember that not all cases are reasonable candidates for tracheal stenting. Tracheal stenting involves the placement of a tube-like structure (ie. stent) into the trachea to push the walls of the trachea outward to allow for air passage. This procedure involves general anesthesia, but is generally very quick and easy to perform. Some immediate relief is expected, however, long-term medications may still be required to control signs.
At this stage, the appropriate size for a stent must be calculated from the fluoroscopic images. Obtaining the proper size for the stent is critical for success. In some cases, placement of the stent requires a second anesthesia and can be done with bronchoscopy or fluoroscopy. Post-procedure radiographs are needed. Appropriate post-operative care is critical to success and includes heavy sedation, cough suppressants, steroids, and antibiotics. Oxygen therapy may be needed in some cases. The dog generally is discharged on 3-6 weeks of a tapering dose of steroids, antibiotics, and cough suppressants.
If a dog has severe respiratory distress associated with tracheal collapse and it cannot be extubated or recovered from anesthesia, a stent can be placed on an emergency basis.
While stents can successfully control debilitating signs associated with intrathoracic tracheal collapse, they are not without risk. Complications of stent placement include collapse, migration, stricture formation, and airway rupture. Follow-up examination with radiographs is required within 1 month, and repeat bronchoscopy should be performed after 4-6 months to detect any problems. Owners must be aware that cough may persist after stent placement.
Nasopharyngeal Balloon and Stent
Nasopharyngeal Stenosis
The nasopharynx is the junction between the back of the nasal passages (region traditionally considered the nose or "muzzle") and the region where the esophagus and trachea begin. When air is breathed in through the nose, it travels through the nasal passages, through the nasopharynx and enters the trachea to be passed to the lungs. Obstruction in this region (stenosis) results in poor or no airflow, which prevents oxygen from being carried to the trachea effectively when the pet's mouth is not open. Signs commonly seen with this condition are sneezing, nasal discharge, constant open-mouth breathing and snoring. Animals may be unable to sleep, eat, or breathe normally unless the mouth is open.
Stents can be placed across the obstruction to permanently open the stenotic area. When stents are in position, air can pass through the nostrils, through the nasopharynx and down to the lungs. This procedure requires general anesthesia and specialized equipment such as computed tomography, fluoroscopy and rhinoscopy. If the stenotic region can be opened sufficiently, an improvement in the clinical signs demonstrated by your pet is expected.
Fluoroscopic and Endoscopic Ureteral Stent
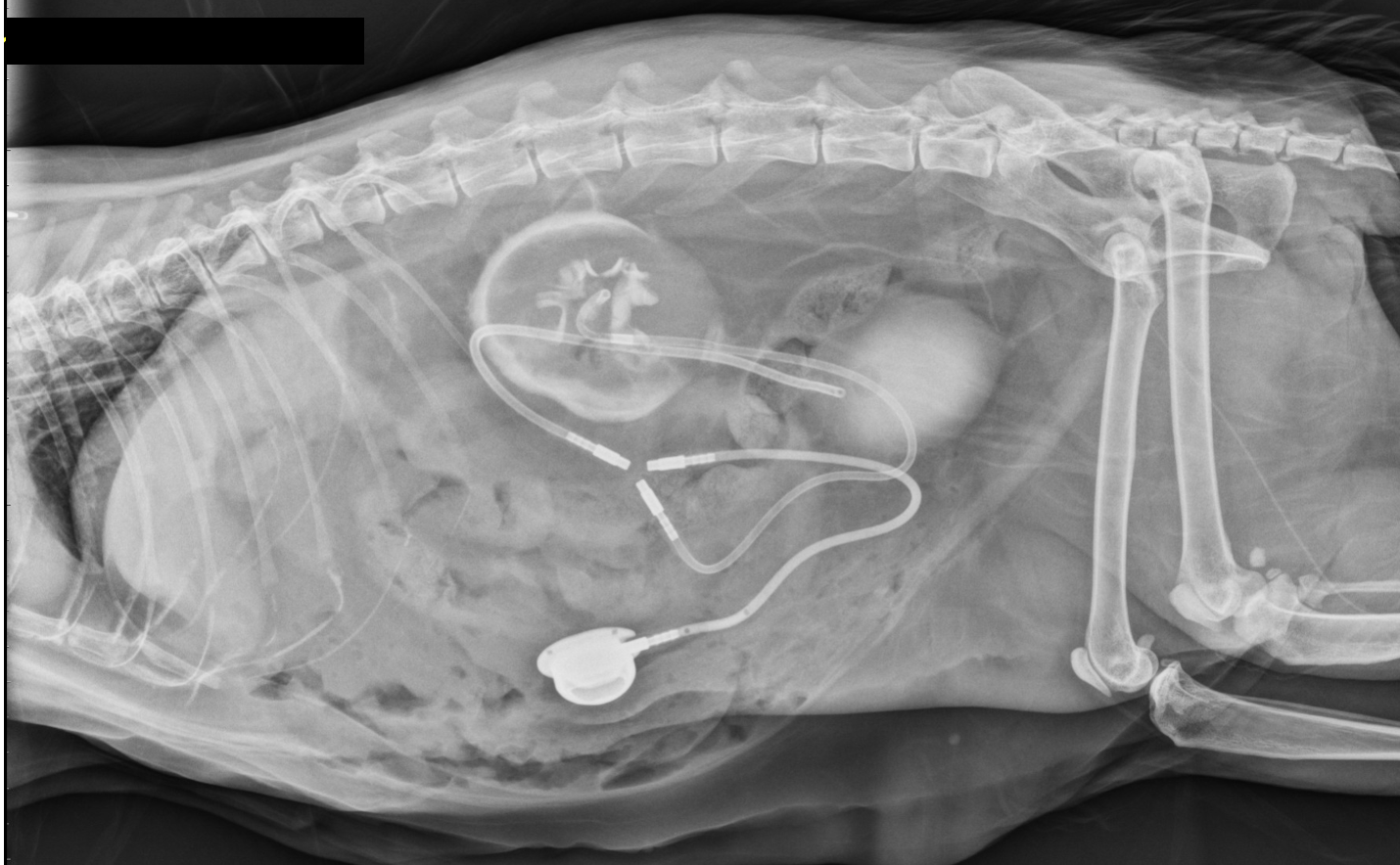
Ureteral Obstruction
Dogs and cats have two ureters. The ureter is the tube connecting the kidney to the bladder and has the responsibility of carrying urine to the bladder after it is formed in the kidney. The ureter can become obstructed by crystals, stones, blood or a combination of these substances. Obstruction can prevent urine from travelling to the bladder which may be a life-threatening condition. Depending on the type of obstruction, surgery may be indicated. Surgery can be successful in many cases, however, surgery is not without complications and may not be indicated in select situations.
Other options for the treatment of ureteral obstructions include ureteral stenting and subcutaneous ureteral bypass. Ureteral stenting involves the placement of a tube within the ureter that extends from the kidney to the bladder to allow for the passage of urine. In ureteral obstructions that occur in dogs, the stent can often be placed with a minimally invasive technique involving the use of a camera that is passed into the bladder. In cats, ureteral stents are placed with a surigical procedure. Subcutaneous ureteral bypass is a procedure where an artificial ureter is created with several tubes. These tubes are designed to allow urine to pass from the kidney to the bladder providing a bypass of the ureter.
Urethral Stent
Urethral Stricture/Non-malignant Obstruction
The urethra is the tube that carries urine from the bladder and expels it outside of the body. When trauma occurs to the urethra or surgery of the urethra is necessary, stricture (decrease in diameter or closing down) can occur. When a complete obstruction occurs, this is a life-threatening emergency, and the affected pet should be evaluated immediately. Opening of the stricture can be performed with a balloon device that causes expansion, but this may not be effective in all cases.
If balloon dilation is unsuccessful, there may be an indication for the placement of a metal or metal-alloy stent that allows for opening of the urethra. The stent pushes outward (against the walls of the urethra) to allow opening of the urethra resulting in the improved ability to urinate.
Tumors of the urethra are seen more commonly than trauma-induced strictures. Please see the page on “Malignant Obstruction” for more information.
Esophageal Stent
Esophageal Obstruction
The esophagus is the organ that carries food from the mouth to the stomach. The esophagus may become closed down due to trauma, previous surgery or chronic irritation from gastric juices. The decrease in esophageal diameter is called a stricture and may result in difficulty of the passage of food into the stomach. Several treatment options are available for esophageal strictures, and an internal medicine specialist can discuss and provide these options to pet owners.
In certain rare cases of strictures that do not respond to traditional therapies, esophageal stenting may be considered. Esophageal stenting involves the placement of a metal or metal-alloy stent that has the capability of opening the esophagus. The purpose of the stent is to improve your pet’s ability to pass food down the esophagus, but other medical management techniques will likely continue to be necessary.
